| Table of Contents |  |
|
Original Article
| ||||||
| Vascular profile of dolichoectasia differs depending on the presenting symptoms | ||||||
| Jose Gutierrez1, Jennifer Carrasquillo2, Gustavo Ortiz3, Clinton B Wright4 | ||||||
|
1MD, MPH, Assistant Professor of Neurology, Department of Neurology, College of Physicians and Surgeons, Columbia University, New York, NY, USA.
2MD, Postdoctoral fellow, Evelyn F. McKnight Brain Institute, Department of Neurology, Leonard M. Miller School of Medicine, University of Miami, USA. 3MD, Assistant Professor of Neurology, Evelyn F. McKnight Brain Institute, Department of Neurology, Leonard M. Miller School of Medicine, University of Miami, USA. 4MD, MS, Associate Professor of Neurology, Departments of Neurology and Epidemiology and Public Health, Leonard M. Miller School of Medicine, University of Miami, USA. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Gutierrez J, Carrasquillo J, Ortiz G, Wright CB. Vascular profile of dolichoectasia differs depending on the presenting symptoms. Edorium J Cardiol 2014;1:1–10. |
|
Abstract
|
|
Aims:
To evaluate the cardiovascular profile of patients with dolichoectasia and compressive versus vascular symptoms.
Methods: We diagnosed patients with dolichoectasia in a hospital-based practice and used Smoker's and Ubogu's criteria to define dolichoectasia of the basilar artery and vertebral arteries, respectively. For the anterior circulation and the posterior cerebral artery, we used two-featured criteria for dolichoectasia consisting of compression of the parenchyma and an aberrant pathway. Results: We identified 18 patients with dolichoectasia of at least one intracranial artery (mean age 56 years, median 61 years, range 32–90 years; eight patients were women, nine patients were Hispanic whites, eight were blacks, and one was white). Two out of three patients who presented with compressive symptoms attributed to dolichoectasia did not have any cardiovascular risk factors. Ten patients presented with vascular symptoms. Six of these patients were men and four were women. Excluding patients with HIV, the remaining six patients with vascular symptoms had a greater number of cardiovascular risk factors (1 to 7 risks) when compared with the group with isolated compressive symptoms (0 to 3 risks). The most affected vessels were the basilar and vertebral arteries, followed by the internal carotid and anterior cerebral arteries. Conclusion: Dolichoectasia and cardiovascular symptoms are more often found in patients who present with vascular symptoms while patients with compression symptoms less frequently have cardiovascular risk factors. The mechanism underlying dolichoectasia in patients with compressive symptoms need to be further investigated. | |
|
Keywords:
Dolichoectasia, Arterial tortuosity, Vascular remodeling, Fusiform aneurysm, Arteriopathy
| |
|
Introduction
| ||||||
|
Dolichoectasia is a disease that affects the arterial wall and results in tortuous, elongated and dilated vessels and has been called by several names including atherosclerotic aneurysm, megadolichoectasia, and fusiform aneurysm [1] [2] [3]. In an initial autopsy series from a large referral center early in the 20th century, the prevalence of dolichoectasia was 0.13% in asymptomatic patients [3]. More recent autopsy series have reported a prevalence of 6% in patients with any neurological disease [4]. Radiological studies have shown a prevalence of 4.8% in patients with compressive cranial neuropathies [5]. The highest prevalence has been reported in patients with stroke (3.1–18.7%) [1] [6]. The etiology of the abnormal dilation of arteries in dolichoectasia is unknown but the strong association with traditional cardiovascular risk factors especially hypertension has suggested a causal link. However, the presence of dolichoectasia in other non-atherosclerotic processes argues against atherosclerosis as the only hypothesis. Dolichoectasia is usually seen in older patients especially hypertensive men [6] [7] [8] but dolichoectasia can be seen at any age and in the absence of atherosclerosis, for example, in polycystic kidney disease, Moya-Moya syndrome, Enhlers-Danhlos syndrome, neurofibromatosis and trauma [9] [10]. The disease predominantly affects the basilar artery (BA) and posterior circulation but the anterior circulation can be involved in up to one-third of patients [2]. A limiting factor in the study of dolichoectasia has been the lack of uniform criteria and a dependence on visual assessment of vessel shape for the identification of dolichoectasia [7]. However, in 1986 Smoker et al. suggested diagnostic criteria for basilar artery dolichoectasia based on the expected course of the basilar artery in relation to surrounding structures [11]. These initial criteria were developed for computed tomography angiography (CTA) of the intracranial circulation, but other authors have used the same anatomical references for brain magnetic resonance imaging (MRI) or magnetic resonance angiography (MRA) [6][8]. For the vertebral arteries Ubogu et al. suggested that a deviation of 10 mm from an imaginary line traced between the entry point of the vertebral arteries (VA) into the intracranial cavity and the origin of the basilar artery, or any portion of the vertebral arteries above the pontomedullary junction, could be considered diagnostic of vertebral arteries dolichoectasia [8]. There are no criteria for anterior circulation dolichoectasia or posterior cerebral artery dolichoectasia. We present a well-characterized study with detailed neuroimaging from a tertiary care center. The goal of our report is to propose tortuosity and compression of the brain parenchyma as additional criteria for the diagnosis of dolichoectasia. | ||||||
|
Materials and Methods
| ||||||
|
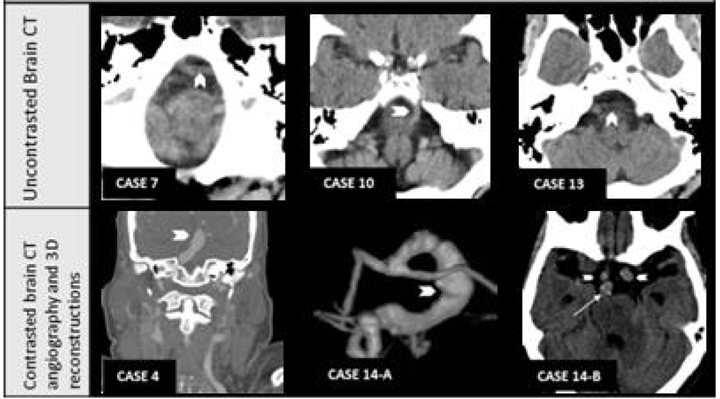
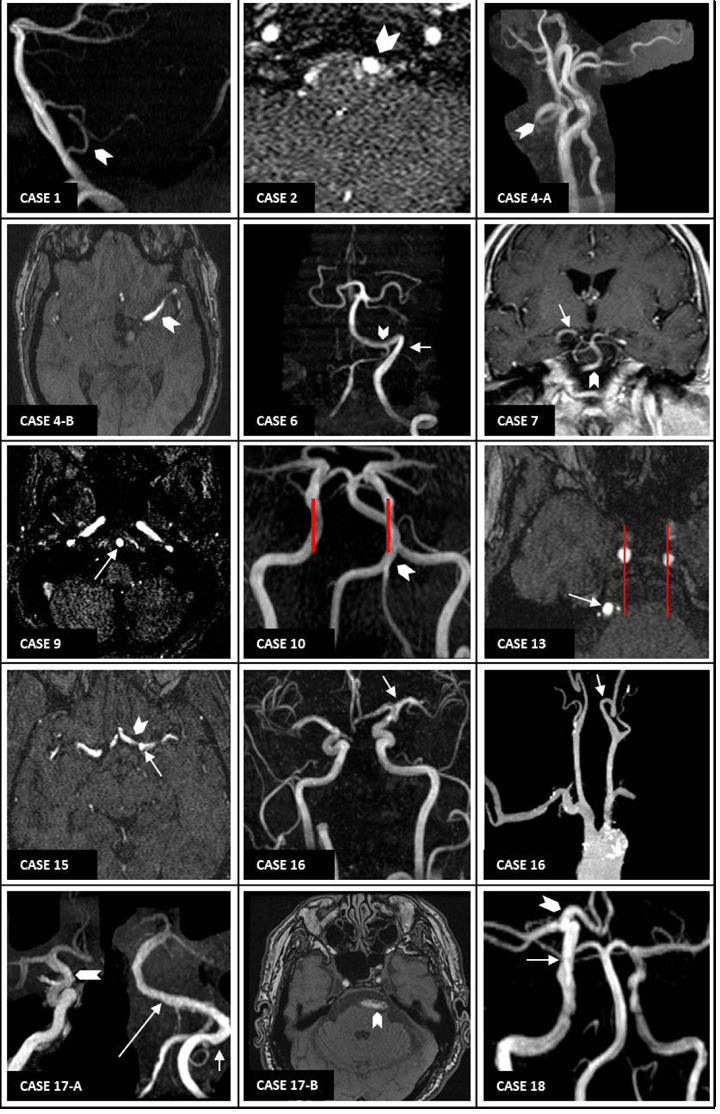
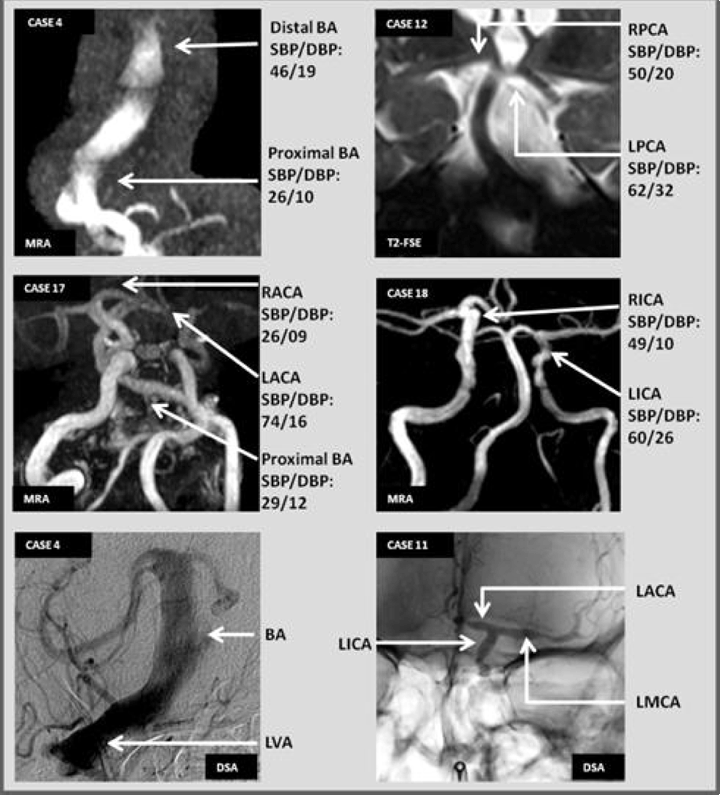
We identified all patients seen by the authors from June 2008 to January 2011 in the neurology inpatient service. We used various imaging modalities to identify patients with dolichoectasia, including non-contrast computed tomography (CT) scan, CTA, MRI scan, MRA, and digital subtraction angiography (DSA) of the head. For the basilar artery, Smoker's criteria were applied. These criteria take into account the diameter, height of the basilar artery bifurcation, and basilar artery lateral deviation relative to the hypothetical midline [11]. We diagnosed dolichoectasia if (i) the basilar artery antero-posterior diameter was >4.6 mm on axial slices using either CTA or MRA images, (ii) if the basilar artery extended to the cerebellopontine angle, or (iii) if the height of the basilar artery bifurcation was at the level of the third ventricle or indenting its floor. The diameters were measured digitally with the embedded tools used by our imaging software provider (iSite Enterprise, Philips Electronics, USA). Additionally, we also considered basilar artery dolichoectasia when the basilar artery silhouette passed the lateral margins of any of the intracavernous internal carotid artery (ICA) silhouettes (Figure 1, Case 10) or when the basilar artery clearly compressed or impinged the brain parenchyma as seen on MRI or CTA (Figure 1, Case 17-B)). The vertebral arteries dolichoectasia was determined using the same criteria as Ubogu et al. mentioned using CTA, MRA or DSA [8]. For the anterior circulation and the posterior cerebral artery (PCA) we used two criteria; tortuosity and compression of the brain parenchyma. Dolichoectasia of the middle cerebral artery (MCA), anterior cerebral artery (ACA), supraclinoid ICA or PCA was present if these two criteria were met. The first step was to evaluate the coronal views of the intracranial circulation CTA or MRA reconstruction; we looked for symmetry of the ICA bifurcation as well as the configuration of the MCA, ACA and PCA on both the sides (Figure 2, Case 16 and Case 18). If a marked asymmetry (suggestive of abnormal elongation of one vessel) was observed, we analyzed axial images to look for compression. The compression criterion was met if brain parenchyma was compressed or impinged upon by the first segment of any of these vessels using CTA, MRI or MRA source images (Figure 1, Case 12 and Case 16). If asymmetric, tortuous vessel shape plus compression of the parenchyma were found, we labeled the artery as dolichoectasia. We did not include secondary or tertiary branches of the MCA, ACA or PCA due to the natural tortuosity of these branches. For the radiological evaluation, we examined vessel configuration using multiple technologies CT scan, MRI scan, MRA, CTA and DSA as available. At first we usually reviewed the non-contrast CT scan of the head. On the axial cuts, it is often possible to observe a dilated or tortuous basilar artery anterior to the brain stem. The relative absence of other structures in the cerebrospinal fluid space at this level facilitates this (Figure 1, first row). However, we did not depend on non-contrast CT scan to diagnose posterior circulation dolichoectasia since contrast studies provide better visualization of the vessels. Suspected anterior circulation dolichoectasia is more difficult to diagnose on contrast CT scan. While using head CTA, we examined axial source images as thin cuts allow visualization of the relationships between vessels and the parenchyma ( (Figure 1, second row. Although the resolution of CT scan is inferior to MRI scan and does not allow high definition of the brain parenchyma, it is possible to determine obvious parenchymal impingement. The coronal and sagittal cuts offer another perspective that can be helpful. Finally, rotating the three-dimensional reconstruction allows the intracranial circulation to be evaluated from multiple angles (e.g. when examining the anterior circulation and the symmetry of the ICA bifurcations as well as the laterality of the basilar artery). The evaluation of dolichoectasia on brain MRI provides more anatomical definition than CT scan and allows better visualization of the vessels and the parenchyma (Figure 3). We use multiple sequences to obtain information on suspected dolichoectatic arteries. The T-2 based sequences provide high contrast between the vessel and surrounding cerebrospinal fluid, although thick cuts can lead to partial volume effects, and gaps between slices can result in missing details. Examining the coronal, sagittal and axial cuts improve visualization of the vessel pathway and its relationship with the parenchyma. For the posterior fossa, especially if suspecting compression of a nerve root by a dolichoectasia vessel, sequences with high-anatomical definition such as T2 three-dimensional constructive interference in steady state (CISS) sequences are ideal [12]. Brain MRAs can be examined in the same way as CTA. (Figure 2) (Figure 3). Additionally, other pathological findings often associated with dolichoectasia such as leukoaraiosis, increased perivascular space (état-criblé) and lacunar stroke can be detected using MRI ( (Figure 3, bottom row) Although DSA was done in five patients, this information did not change our impression in any case (Figure 4, bottom row), although measurement of the arterial diameters is likely to be more accurate in angiography than with CTA or MRA. However, we did not systematically use DSA images to measure the basilar artery diameter. Major cardiovascular risk factors were defined as male sex, age >55 years in men and >65 years in women, a family history of premature cardiovascular disease, hypertension, diabetes mellitus, dyslipidemia, smoking or the presence of coronary artery disease (CAD) or its equivalents. The local Institutional Review Board approved the study. | ||||||
|
| ||||||
|
| ||||||
|
| ||||||
|
| ||||||
|
| ||||||
|
| ||||||
|
| ||||||
|
Results | ||||||
|
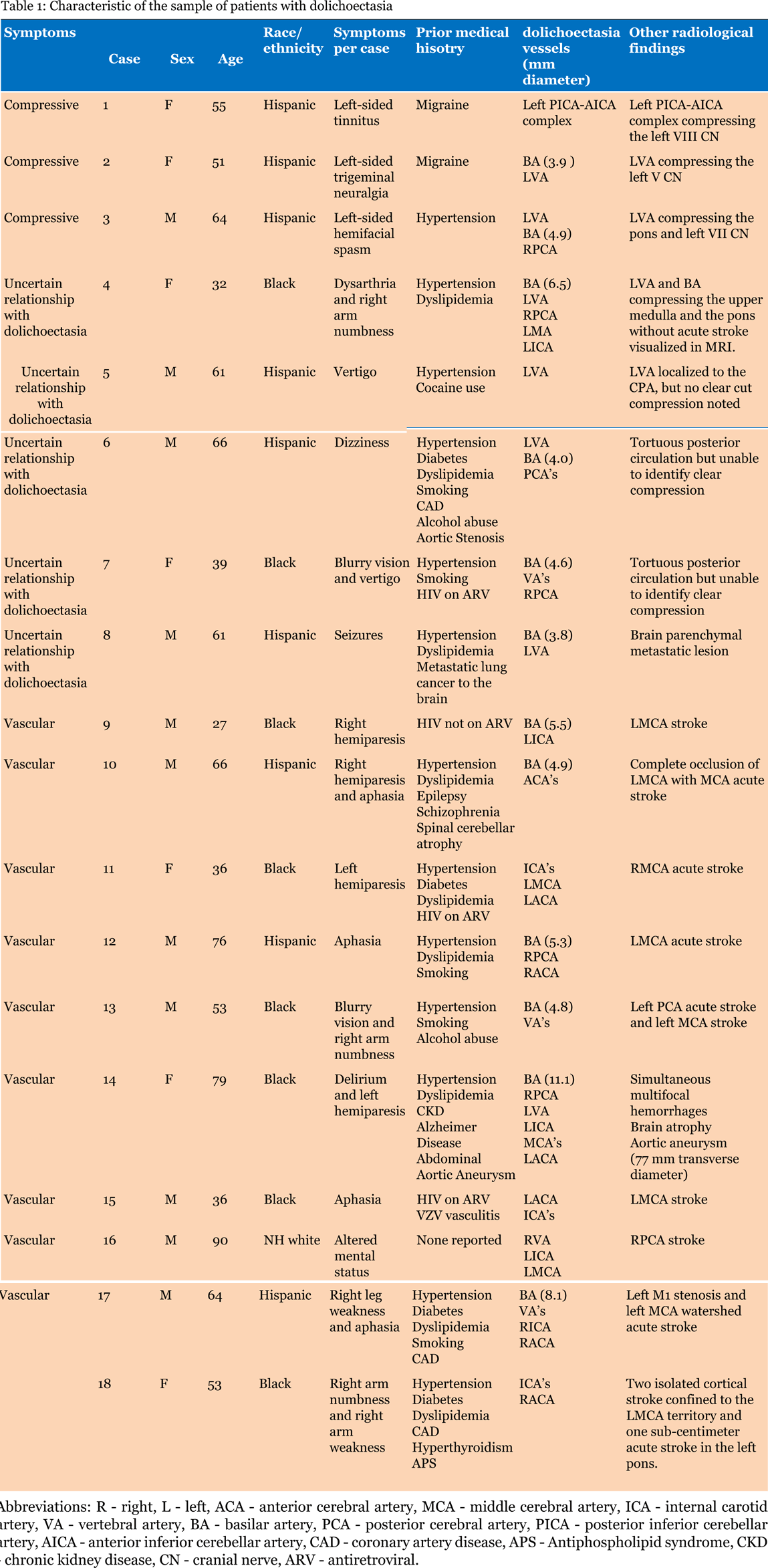
We found 18 patients with dolichoectasia of a least one intracranial artery. The characteristics of the sample are given in Table 1. Three patients presented with compressive symptoms and ten with vascular symptoms, Only six out of the ten patients with vascular symptoms had the symptoms in the same distribution as the dolichoectatic vessel. Five patients had a presentation that was difficult to attribute only to a vascular or compressive manifestation. Two out of the four patients with HIV were diagnosed with HIV vasculopathy and one with Varicella-Zoster vasculitis Table 1. Two out of three patients who presented with compressive symptoms attributed to dolichoectasia did not have any cardiovascular risk factors. These two patients were females and both had migraine with aura. One had trigeminal neuralgia and the other vertigo. In all cases, the symptoms were stable and they were not associated with typical migraine. The third patient with isolated compressive symptoms had left hemifacial spasm attributed to basilar artery dolichoectasia. In five patients, we could not attribute the symptoms to either compression of the dolichoectasia artery or vascular disease in the area of the symptoms. These patients had a profile much more similar patients with pure vascular symptoms (i.e, more cardiovascular risk factors) than the patients without vascular symptoms. The ten patients with dolichoectasia and vascular symptoms were older than those without. The patients with HIV were the youngest in this group. Six of these patients were men and four were women. Excluding patients with HIV, the remaining six patients with vascular symptoms had a greater number of cardiovascular risk factors (risk factors 1–7) when compared with the group with isolated compressive symptoms (risk factors 0–3). One of the nine cases presented with multifocal parenchymal hemorrhages, coexistence of an aortic aneurysm and a very severe forms of dolichoectasia. This case has been reported in detail elsewhere (Figure 1, Case 14)[13]. The basilar artery was affected in 11 patients; the same number had affected in vertebral arteries dolichoectasia (right, left or both). The ICA (right, left or both) was affected in eight patients, and the ACA was affected in the same number of patients. The PCA's were dolichoectatic in six patients, the MCA's in four, and only one patient had a dolichoectatic AICA-PICA complex (Table 1). Isolated posterior circulation dolichoectasia was the most common presentation (eight patients) compared with the isolated anterior circulation dolichoectasia (three patients). Both territories were affected in seven patients. The antero-posterior basilar artery diameter had a mean of 5.2 mm (median 4.9 mm, range 3.8–9.8 mm). Only two patients had a basilar artery diameter below the 4.5 mm Smoker's criteria threshold and both had isolated compressive symptoms and no traditional cardiovascular risk factors. Four patients had Trancranial Doppler (TCD) as part of their stroke workup. When contrasting the arterial pressures of the dolichoectasia vessels against the non-dolichoectasia vessels in the same patients the pressures were lower on the affected side. Additionally, largely dilated vessels have dampening of the flow with very low diastolic pressures suggestive of poor elastic recoil in these dilated arteries (Figure 4). Transcranial Doppler monitoring of the MCA ipsilateral to a dilated ICA was done in one instance only (Case 18) and no microembolic signals were detected. | ||||||
| ||||||
|
Discussion
| ||||||
|
Dolichoectasia is a disease of the arterial wall, characterized by dilatation, tortuosity and elongation of affected vessels [1] [3][6][8][14]. In this case series, we present examples of this condition with associated pathology, illustrating the breadth of dolichoectasia presentations. We also provide a multimodal approach for the diagnosis of dolichoectasia. While dolichoectasia has traditionally been considered a bystander in the presence of vascular disease, mainly atherosclerosis, these assumptions need to be revisited [4] [14] [15]. Increased recognition of dolichoectasia and its associated manifestations is one of the first steps in this process. Reproducible and objective criteria have been missing and have hampered the ability of different groups to compare populations. We found a wide spectrum of diseases associated with dolichoectasia in this series. In cases where a dolichoectasia vessel compresses a nerve root and causes symptom, a direct mechanical effect is likely to blame. This occurred in three of our patients. However, none of our patients underwent surgical interventions with relief of symptoms that might have proven that dolichoectasia was the cause in these cases. Nevertheless, other authors have presented cases with symptom improvement after surgical nerve decompression [16]. Tortuosity of the vessels can be seen in trauma, [17] congenital or acquired variants of the brain arterial configuration, inherited metabolic disorder, etc.[9] [17] [18] [19] The role of dolichoectasia in vascular diseases complex, but dolichoectasia in this context is most likely a function of progressive arterial dilatation [8] [20] [21]. Determining the underlying cause is difficult in cases with vascular diseases and this uncertainty is reflected in the large number of cases where we could not attribute a direct role of the dolichoectasia vessel to the patient's symptoms. Further, even in cases where we determined a link between dolichoectasia and vascular disease, our cross-sectional design precludes causality inferences. While prospective data regarding the link between dolichoectasia and vascular disease are lacking, many studies have linked dolichoectasia with cardiovascular risk factors and cardiovascular diseases [3] [15][22]. Cohort studies have shown a greater risk of vascular events in patients who have progression of the dolichoectasia (defined as progressive dilatation of the arteries) compared with those who remain stable, suggesting that dolichoectasia could be a modifiable risk factor for stroke once prevention measures are identified [20] [21]. Some proposed mechanisms for vascular events include mechanical traction of branching arteries, [23] dampening of the blood flow due to dilatation, [24] artery-to-artery embolism due to mural thrombosis, arterial occlusion due to insitu thrombosis [25] or intramural hemorrhage [26]. In the four patients who underwent TCD in our series, all had low flow velocities in the dolichoectasia vessels compared with the non-dolichoectasia vessels suggesting hemodynamic changes worthy of further study. Vascular remodeling is thought to cause dilatation due to complex interactions between flow mechanics and the arterial wall [14] [27]. These interactions can also theoretically be modulated by genetic and environmental factors. Considering the relatively low level of evidence of most dolichoectasia studies, these pathophysiological underpinnings are difficult to confirm. It is interesting to note that HIV infect the muscularis layer of arteries and leading to weakening of the arterial wall, in some cases lead to arterial dilatation and stroke [28]. Also, patients with metabolic diseases that affect collagen and elastin integrity often have weak arterial walls, and they too present with symptomatic dilated and tortuous intra and extracranial vessels [10] [19]. In patients with atherosclerosis, it seems that the endothelium plays an important role in the weakening of the muscularis layer due to a cascade of trophic factors that cause disruption of the internal elastic lamina and overexpression of metalloproteinases (MMP) with subsequent cleavage of the elastic tissue and thinning of the media layer [27] [29]. We used Smoker's criteria and Ubogu's criteria for the vertebral arteries and the basilar artery [8] [11]. The core principle of the criteria is to contrast the expected versus the observed pathway of an artery to gauge the degree of abnormality, aided by stable anatomical landmarks such as bony structures. Smoker's criteria also include compression of the surrounding structures as a marker of abnormal vessel trajectory. There are no established criteria to assess dolichoectasia in the anterior circulation or the PCA's. We attempted to systematically evaluate our cases for anterior circulation dolichoectasia, using parenchymal compression and aberrant vessel trajectory (often compared to the contralateral vessel) as criteria for dolichoectasia in the ICA, MCA, ACA and PCA. Using compression as a criterion for dolichoectasia in the anterior circulation is justified as almost all reports involve symptomatic compression of surrounding structures [2] [16][18][22]. The larger dimensions of the cranial cavity in relation to anterior circulation vessels, and the fact that a large proportion of those vessels are supratentorial, makes it more difficult to use bone as a reference. This may well explain why dolichoectasia has been under-reported in the anterior circulation [14]. We acknowledge a number of limitations. Our sample is subject to referral bias due to the tertiary nature of our academic center. Our goal was to present clear cases of dolichoectasia to illustrate the wide variety of presentations that can be seen rather than including every case where the diagnosis might be questionable. It is also possible we could have missed subtle cases. Further, asymptomatic cases of dolichoectasia, as well as more mild forms of the disease that might not have prompted us to search, are underrepresented in our series. The diagnostic criteria of the anterior circulation and the PCA's have been used in a large, population-based study that sought to compare different diagnostic methods of dolichoectasia [30]. The validity of these various methods will need to be further validated by others with their usefulness in predicting outcomes. Future directions in the study of dolichoectasia should include its objective definition using arterial diameter parameters obtained from population-based samples as well as prospective cohorts with research questions clearly aimed at filling the gaps in knowledge of this interesting and understudied arterial disease. | ||||||
|
Conclusion
| ||||||
|
Dolichoectasia and cardiovascular symptoms are more often found in patients who present with vascular symptoms while patients with compression symptoms less frequently have cardiovascular risk factors. The mechanism underlying dolichoectasia in patients with compressive symptoms need to be further investigated. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Jose Gutierrez – Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Jennifer Carrasquillo – Acquisition of data, Critical revision of the article, Final approval of the version to be published Gustavo Ortiz – Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published Clinton B Wright – Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Jose Gutierrez et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Authors
| |||
| |||