| Table of Contents |  |
|
Case Report
| ||||||
| Livin' Livedo Loca: Cholesterol embolization syndrome secondary to cardiac angiography | ||||||
| Nicholas Kevin Laidler | ||||||
|
MBBS (Hons); BSc (Physio)
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Laidler NK. Livin' Livedo Loca: Cholesterol embolization syndrome secondary to cardiac angiography. Edorium J Cardiol 2015;2:4–8. |
|
Abstract
|
|
Introduction:
Cholesterol embolization syndrome is a rare but well recognized cause of organ disease. There is no specific therapy for the disorder and treatment is comprised around the supportive care of existing end organ damage and secondary prophylaxis against subsequent episodes of cholesterol embolization.
Case Report: A case of a 68-year- old female with a history of ischemic heart disease, diabetes, supraventricular tachycardia, hypercholesterolaemia and diverticulitis who presented to hospital twice in three days with two different complaints, abdominal pain and then chest pain. The abdominal pain was dismissed as diverticular pain in lieu of any other evidence and a NSTEMI was found to be the cause of her chest pain. An angiogram was subsequently performed which precipitated an embolic shower causing end organ damage and providing a pathological basis for the patients initial presentation of abdominal pain. Conclusion: Due to its non-specific presentation cholesterol embolization syndrome is frequently misdiagnosed and undetected. High clinical suspicion is the key to diagnosis. | |
|
Keywords:
Angiography, Atheromatous embolization, Blue or Purple toe syndrome, Cholesterol crystal embolization, Complication
| |
|
Introduction
| ||||||
|
Trauma to the aortic wall during peripheral endovascular interventions can potentially dislodge cholesterol rich atherosclerotic plaques which can then embolize to distal arteries. This process has many names in literature including atheromatous embolization, cholesterol embolism, cholesterol crystal embolization, Blue or purple toe syndrome and cholesterol emboli syndrome which has led to fragmentation of the knowledge base. It can present with subtle or catastrophic manifestations and may mimic other diseases. As a result of its non-specific clinical picture cholesterol embolization syndrome is frequently misdiagnosed or undetected, with diagnoses frequently being made post-mortem. A high clinical suspicion is the key to diagnosis. Its early recognition followed aggressive management including risk factor modification, prevention of further insults, avoidance of predisposing factors, supportive treatment and the removal of the source for the atheroembolism, may help to prevent end organ damage and improve overall clinical outcomes. | ||||||
|
Case Report
| ||||||
|
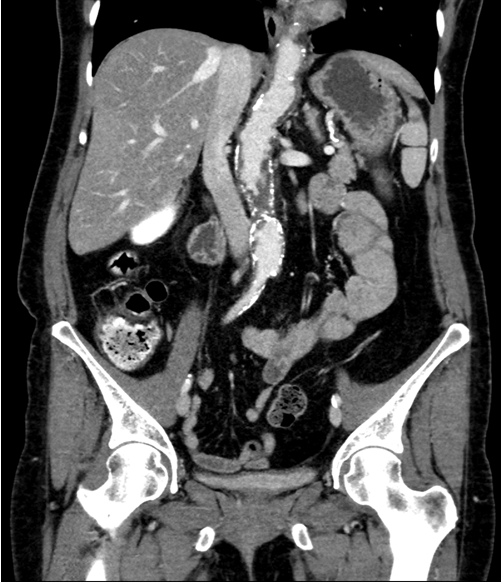
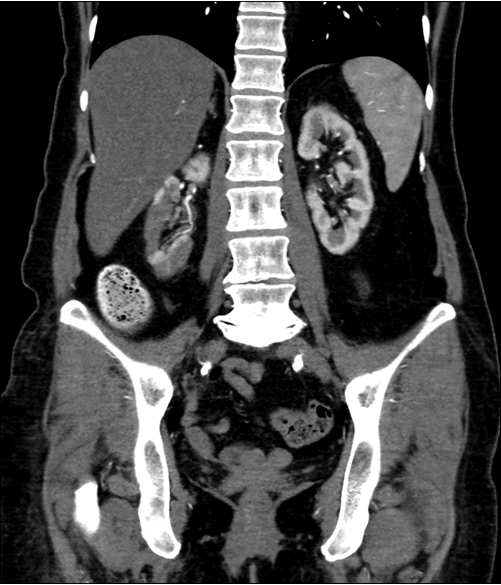
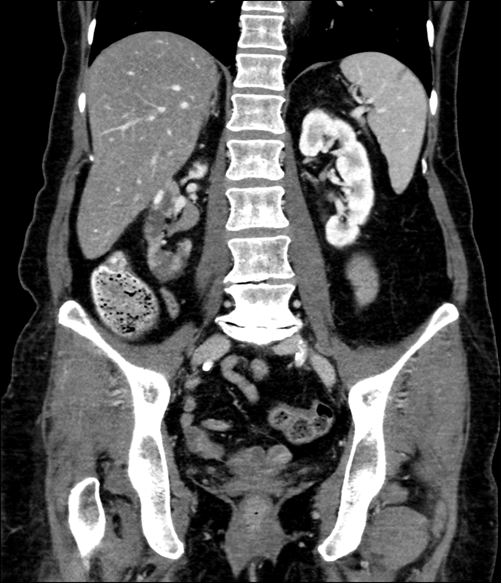
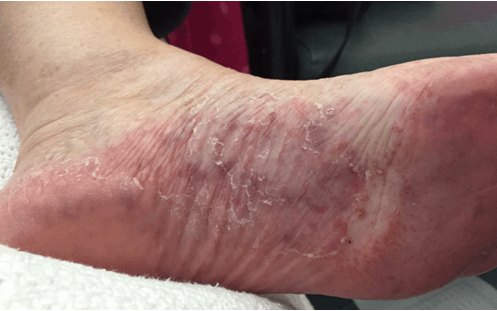
A 68-year-old Caucasian female initially presented to the emergency department of a major hospital with a one day history of acute onset left sided abdominal pain. Her bowels were opening normally and there was no diarrhea. She reported one episode of vomiting and had documented fevers. She was admitted under a surgical team and received an abdominal ultrasound scan and computed tomography scan with no abnormalities detected. On day-two of her admission, she was pain free and was discharged home. The patient re-presented to hospital the following day with sudden onset chest pain and palpitations. She was diagnosed in the emergency room with supraventricular tachycardia (SVT) and cardioverted with 6 mg of adenosine. The pain remained and was located in the left parasternal region radiating to the neck through to her back. There was no history of sweating, palpitations, orthopnea or paroxysmal nocturnal dyspnea. Serial troponins were positive at 0.98 (n =< 0.05) and an ECG indicated a NSTEMI. Her medical history included ischemic heart disease, type two diabetes, hypercholesterolemia, multiple episodes of SVT requiring cardioversion and diverticulitis. HDL and LDL cholesterol levels were 1.1 and 6.4 mmol/L, respectively. The patient had trialled multiple statins but was non-compliant due to statin myopathy. She was taking fenofibrate 45 mg for her hypercholesterolemia. Other medications included diltiazem 150 mg, glicazide 30 mg and aspirin 100 mg. The patient has 45 pack-year history of smoking. There was a significant family history for cardiovascular disease including a maternal myocardial infarction at 51 and a paternal myocardial infarction at 61. The patients' sister also had an MI at age 49 and suffered with SVT. Both the parents suffered with diabetes. There was no history of familial hypercholesterolemia. The vital signs of the patient were stable and within normal limits. The patient was afebrile. Examination reviled no peripheral stigmata of cardiovascular disease or evidence of cutaneous manifestations. JVP was not elevated and there was no central or peripheral cyanosis. Heart sounds were dual with no added sounds or murmurs. The apex beat was not palpable and there were no thrills or heaves. Abdominal auscultation revealed a para-umbilical abdominal bruit. A coronary angiogram was performed which reported 100% RCA stenosis, 40% prox/mid LAD stenosis and 50% stenosis in the 1st diagonal which was medically managed. Following the angiogram the patient reported a return of abdominal pain, this time right sided and radiating through to the back. An abdominal CT scan was requested which demonstrated severe atherosclerosis in the abdominal aorta (Figure 1) embolic phenomenon and acute infarcts were seen in the kidneys (Figure 2) and spleen (Figure 3). It was thought that this was likely secondary to an aortic cholesterol thrombotic plaque shower that may have been precipitated by the angiogram. A lactate of 15 was returned at this time, creatinine rose to 112 umol/L (baseline of 77 umol/L) and eGFR reduced to 46 mL/min/1.73 m2 (baseline 65 mL/min/1.73 m2). Five days later livedo reticularis was demonstrated on the sole and medial aspect of the left foot (Figure 4). The patient was managed conservatively with supportive therapy and discharged home on a higher dose of fenofibrate, low dose statin, advice on implementing a low cholesterol diet and dual antiplatelet therapy. In hindsight it was likely that Mrs WS's initial presentation for abdominal pain was caused by mesenteric ischemia which is related to her significant atherosclerotic disease. | ||||||
| ||||||
|
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Cholesterol embolization syndrome is caused by showers of cholesterol plaques from large arteries with atheromatous disease. Atheromatous embolization most commonly originates from the abdominal aorta [1] [2] [3][4]. Emboli normally occlude smaller arteries (100––300 µm in diameter) and arterioles distal to this site [4] [5][6][7]. These emboli occlude distal small arteries causing ischemia, gangrene and necrosis. Cholesterol emboli not only mechanically occlude the vessel but also trigger an inflammatory reaction that eventually causes endothelial proliferation and eventually fibrosis [4][8]. Cap rupture is a prerequisite of cholesterol embolization syndrome. The cap may be destabilized from within the plaque via an inflammatory process or from its luminal side by traumatic disruption during a vascular procedure [4] [5]. Cholesterol embolization syndrome may occur spontaneously. However, there are a number of precipitating factors that enhance a patient's risk. These include invasive procedures such as angiography, endovascular interventions, vascular or cardiac surgery, trauma and anticoagulation [1] [3][9]. Cholesterol embolization syndrome is inextricably linked to the general development of atherosclerosis. It therefore shares the same risk factors as general atherosclerosis, which include; a positive family history, male sex, hypercholesterolemia, tobacco use and systemic hypertension [7] [8]. The exact incidence of cholesterol embolization syndrome is unknown[[4] [5]. It is, however, more commonly seen as a complication of invasive procedures, involving large calibre vessels with atherosclerotic disease [10] [11][12][13][14]. As upper limb vessels have a lower incidence of atherosclerotic disease than the upper limb trans-femoral procedures such as coronary angiography carry a higher risk of cholesterol embolization syndrome [7]. The incidence of non-iatrogenic atheroembolism reported on routine autopsy ranges from 0.15% to 3.4% [1] [11]. However, in patients with known severe atherosclerosis the incidence increases from 8.6% to 12.3% [5] [15]. A prospective study by Fukumoto et al. evaluated patients who underwent left heart catheterization in Japan [16]. Cholesterol embolization syndrome was found to have occurred in 1.4% of the study participants [16]. Cross found a 1.9% incidence of renal failure as a manifestation of cholesterol embolization syndrome after cardiac catheterization [12]. This varies greatly however with Drost et al. finding a 0.002% incidence of cholesterol embolization in their review of 4587 cardiac catheterizations [1]. Aortic catheters or guide wires can cause mechanical trauma and dislodge atheromatous material from the arterial wall. Eggebrecht et al. evaluated the frequency of atherothrombotic material retrieved during placement of coronary catheters and found that 0.5% patients had macroscopically visible atherothrombotic debris [2]. A wide range of clinical manifestations can appear depending on the site of embolic deposition. In its mildest form, cholesterol emboli can be subtle and may go completely unrecognized. However, when there is repeated showering, the result can be disastrous [17]. The clinical features of cholesterol embolization syndrome are most commonly cutaneous, renal, gastrointestinal and neurological [7][8]. The distal extremities are only involved if the site of origin of the atheroma is below the renal arteries [18] . Clinically, patients may report constitutional symptoms such as fever, anorexia, weight loss, fatigue and myalgia [3] [4] [19]. Biochemically signs of systemic inflammation such as anemia, thrombocytopenia leukocytosis, high erythrocyte sedimentation rate, elevated levels of C-reactive protein and hypocomplementemia may be found [3][4] [19]. Cutaneous abnormalities are usually the earliest clinical findings of atheromatous emboli and may appear days to weeks after the provoking event and are seen in approximately 35% of patients [20]. They include livedo reticularis, cyanosis, ulceration, nodules, papura and gangrene [20]. Subcutaneous nodules may also be seen and represent an inflammatory reaction to the surrounding cholesterol crystals [19]. When there is kidney injury secondary to cholesterol embolization a decrease in glomerular filtration rate and a rise in creatinine is commonly seen. However, this too may take weeks to occur [3] [20]. 15% to 20% of patients will have involvement of one or more digestive organs with the most common features being abdominal pain, diarrhea, and gastrointestinal blood loss [19]. Occasionally, bowel infarction and perforation occur [19]. Pancreatitis and adrenal insufficiency are rare but potential causes of cholesterol embolization syndrome [5]. Depending on where emboli deposit, a wide range of neurological manifestations can be seen which range from transient ischemia attacks to paralysis [4][5] [7]. There is no specific therapy for cholesterol embolization syndrome with treatment consisting of supportive care and secondary prophylaxis against further episodes [4][5]. Cholesterol embolization syndrome can be viewed as a manifestation of atherosclerosis and as such risk factor modification forms an integral part of treatment [4] [19]. This includes cessation of smoking, lowering of serum cholesterol, and control of hypertension and diabetes mellitus [4] [19]. Additionally, the avoidance of precipitating factors, the use of protection devices during endovascular procedures and modification of surgical techniques are all considerations that must be introduced in high risk patients [3] [16]. A number of medications have been tried and several have been reported beneficial in the treatment of cholesterol embolization syndrome. Corticosteroid use is still controversial and largely of a theoretical interest [5]. It is postulated to decrease the associated local and systemic inflammatory reactions [5]. The role of statins in atheroembolism remains uncertain. The protective benefit is most likely due to plaque stabilization, anti-inflammatory and immunomodulatory properties [5] [17]. Anticoagulation is not indicated in the treatment of cholesterol embolization syndrome and in fact may worsen the existing disease process [4][5] [7]. It is hypothesized that anticoagulation may prevent thrombus formation over unstable atherosclerotic plaques allowing exposed cholesterol crystals to embolize [4] [5]. Another hypothesis states that these agents may initiate the disruption of a complex plaque by causing intraplaque hemorrhage and subsequent embolization [4]. | ||||||
|
Conclusion
| ||||||
|
During peripheral endovascular interventions trauma to the aortic wall may occur. As a result cholesterol rich atherosclerotic plaques may be dislodged and embolize distally. These may be subtle in presentation or mimic other diseases. Due to its non-specific presentation cholesterol embolization syndrome is frequently misdiagnosed and undetected. High clinical suspicion is the key to diagnosis. Early recognition and aggressive management may prevent end organ damage and improve clinical outcomes. | ||||||
|
Acknowledgements
| ||||||
|
I am thankful to Dr. Jenny Deague for her assistance in this case. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Nicholas Kevin Laidler – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Nicholas Kevin Laidler. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|