| Table of Contents |  |
|
Original Article
| ||||||
| Short-term and long-term outlook after eventually successful albeit transiently complicated percutaneous coronary intervention for chronic total occlusion: The Rivoli chronic total occlusion registry | ||||||
| Andrea Gagnor1, Ferdinando Varbella1, Francesco Tomassini1, Sara Giolitto1, Cristina Rolfo1, Emanuele Tizzani1, Enrico Cerrato1, Alfonso Gambino1, Elisa Favro1, Rosario Tripodi1, Maria Cristina Rosa Brusin1, Paolo Gyai Pron1, Mariangela Peruzzi2, Giuseppe Biondi-Zoccai2,3 | ||||||
|
1MD, Division of Cardiology, Rivoli Hospital, Rivoli, Italy.
2MD, Department of Medico-Surgical Sciences and Biotechnologies, Sapienza University of Rome, Latina, Italy. 3MD, Department of AngioCardioNeurology, IRCCS Neuromed, Pozzilli, Italy (GBZ). | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Gagnor A, Varbella F, Tomassini F, giolitto S, Rolfo C, Tizzani E, Cerrato E, Gambino A, Favro E, Tripodi R, Brusin MCR, Pron PG, Peruzzi M, Biondi-Zoccai G. Short-term and long-term outlook after eventually successful albeit transiently complicated percutaneous coronary intervention for chronic total occlusion: The Rivoli chronic total occlusion registry. Edorium J Cardiol 2016;3:13–21. |
|
Abstract
|
|
Aims:
We aimed to appraise the outlook of successful albeit transiently complicated percutaneous coronary intervention (PCI) for chronic total occlusion (CTO). Percutaneous coronary intervention of CTO may improve symptoms, systolic function and prognosis, but may be associated with short-term complications.
Methods: Baseline, procedural and outcome details on patients in whom CTO PCI was attempted between 2003 and 2012 at our institution were retrieved. We compared those with failed PCI (F group) to those with successful and uncomplicated PCI (SU group) and those with eventually successful albeit transiently complicated PCI (SC group). Results: A total of 435 patients were included, with 25.7% failures and 74.3% successes, including 67.8% in the SU group and 6.4% in the SC group. One-month major adverse cardiac events (MACE) occurred in 0.4% patients in the SU group, 7.1% in the SC group, and 2.7% in the F group (p=0.005). Risk of major adverse cardiac events (MACE) after one month was similar in patients in the SU and SC groups, with both groups faring better than those in the F group (respectively 23.7%, 17.9%, and 18.8%, p = 0.477). Similar trends for >1-month events were found for death and myocardial infarction (both p > 0.05), whereas repeat revascularization was more common after SU group (19.3% versus 14.3% and 6.3%, p = 0.005). Stent thrombosis was more common in SC group (0 versus 7.1% and 1.8%, p < 0.001). Conclusion: Patients with uncomplicated CTO recanalization are at higher risk of restenosis and revascularization, whereas those with final success despite complications are at higher risk of stent thrombosis. | |
|
Keywords:
Chronic total occlusion, Complication, Coronary artery disease, Failure, PTCA
| |
|
Introduction
| ||||||
|
Coronary chronic total occlusion (CTO) is defined as the presence of thrombolysis in myocardial infarction (TIMI) 0 flow with a coronary occlusion dating at least three months [1], and is encountered in 15–30% of all patients referred for coronary angiography [2] [3]. Several retrospective studies have shown that successful CTO revascularization is associated with improvements in symptom burden [4], left ventricular ejection Fraction (LVEF) [5], and survival [6] [7][8]. Yet, percutaneous coronary intervention (PCI) is still attempted only in a minority of CTO [9], mainly because of technical complexity and perceived risk of complications. Success rates for CTO are indeed significantly lower than those for non-CTO lesions, but new techniques (e.g., parallel wire and retrograde approaches) and novel dedicated devices have increased success rate up to 85% or more [10] [11] [12][13]. Procedural complexity seems not to be related with worse in-hospital outcome, as recently reported rates of in-hospital major adverse cardiac events (MACE) for CTO PCI appear similar to those associated with non-CTO PCI patients, at least in selected patients [3]. Yet, the increased risk of peri-procedural complications when CTO PCI is attempted, such as vessel dissection, wire perforation, vessel rupture, contrast nephropathy and radiation injury, is unquestionable. For instance, the retrograde approach has increased procedural success but has introduced specific complications such as donor vessel injury (ischemia and thrombosis) and collateral loss. Despite several reports assessing CTO PCI complications in general, very little is known about relation between success, procedural complications and prognosis. The aim of the present study was to investigate the in-hospital and long-term clinical outcome of patient with eventually successful albeit transiently complicated PCI for CTO in contemporary practice, comparing such cases with successful and uncomplicated CTO PCI or unsuccessful CTO PCI. | ||||||
|
Materials and Methods
| ||||||
|
Study design and patient population Patients and procedures Blood draws for serum creatinine, CK-MB and troponin I were obtained before the procedure, 6–8, 12 and 24 hours afterwards. In, absence of clinical indication for a prolonged hospital observation, subjects were discharged 24–48 hours after the procedure. Follow-up was performed with clinical evaluation at 30 days, 6 months and 1 year and then every year. Stress test (ideally radionuclide techniques or dobutamine stress echocardiography) was performed after 6–8 months. Clinical status at follow-up was evaluated by an independent cardiologist. Definitions and endpoints Given the purpose of our work to focus on different types of CTO PCI, we distinguished patients with failed PCI (F group), from those with successful and uncomplicated PCI (SU group) and those with eventually successful albeit transiently complicated PCI (SC group). Statistical analysis | ||||||
|
Results | ||||||
|
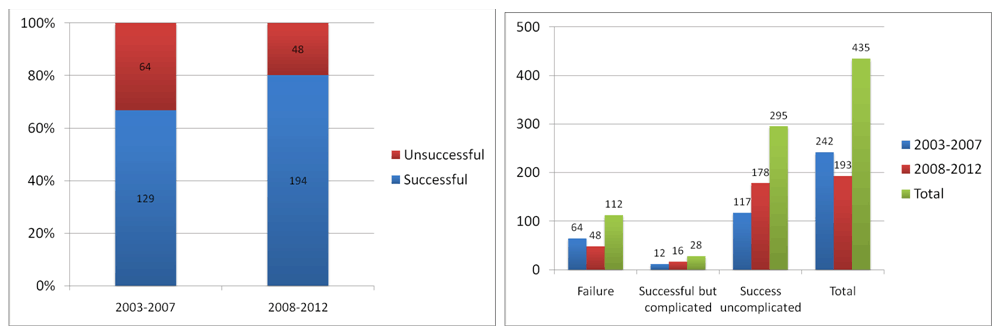
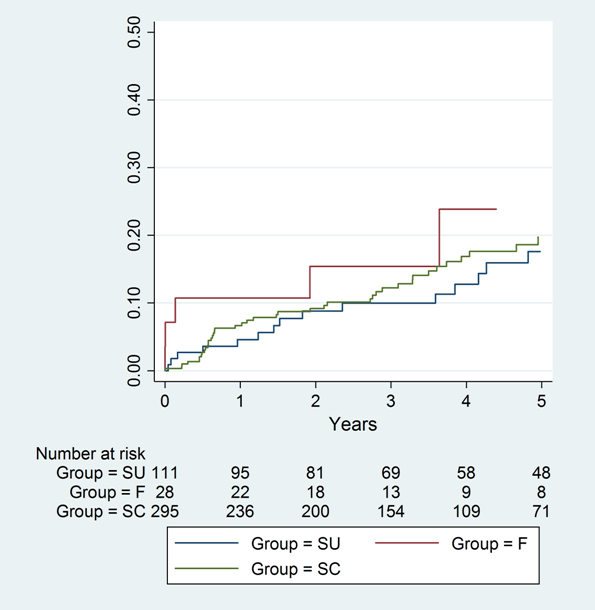
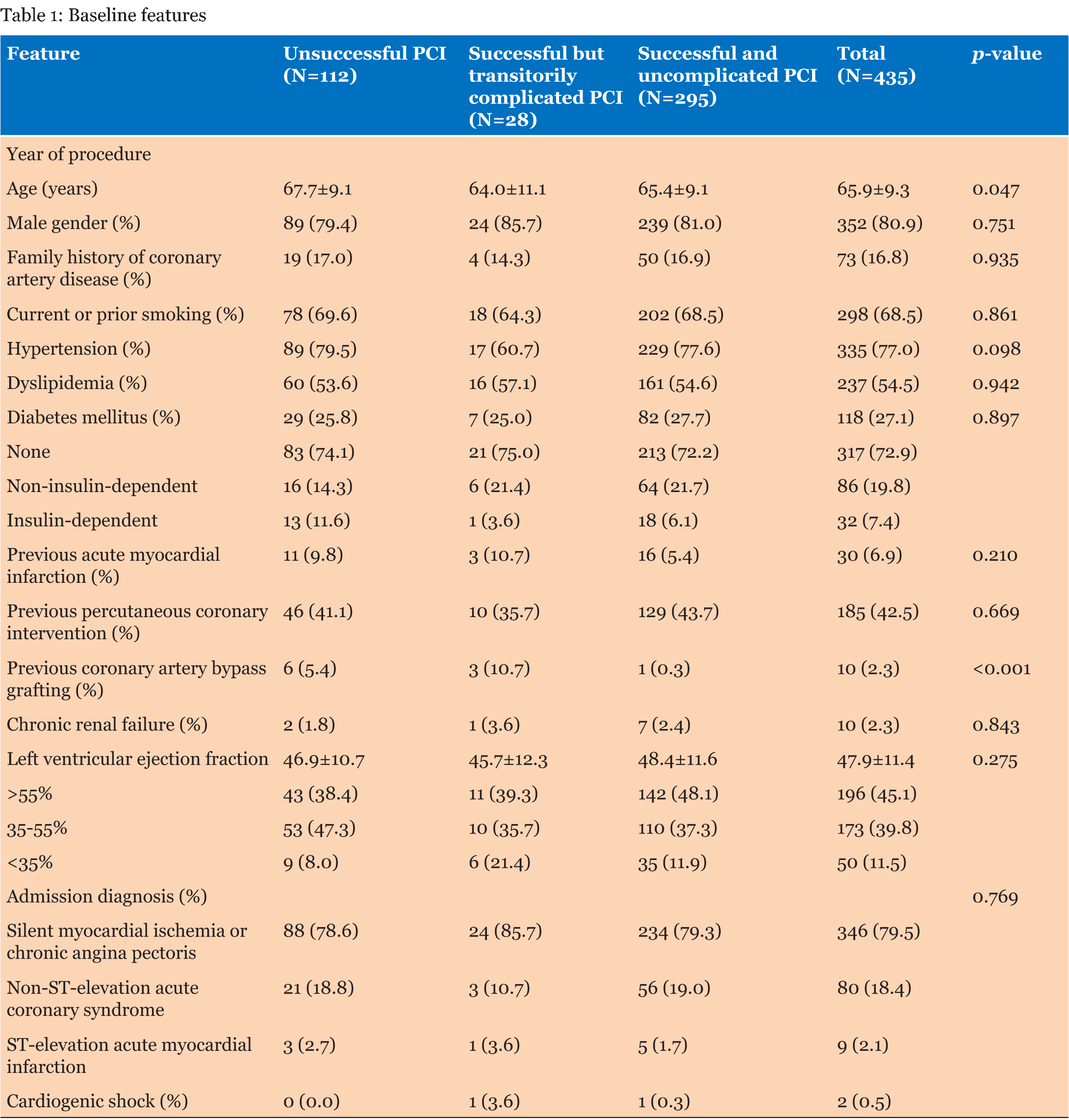
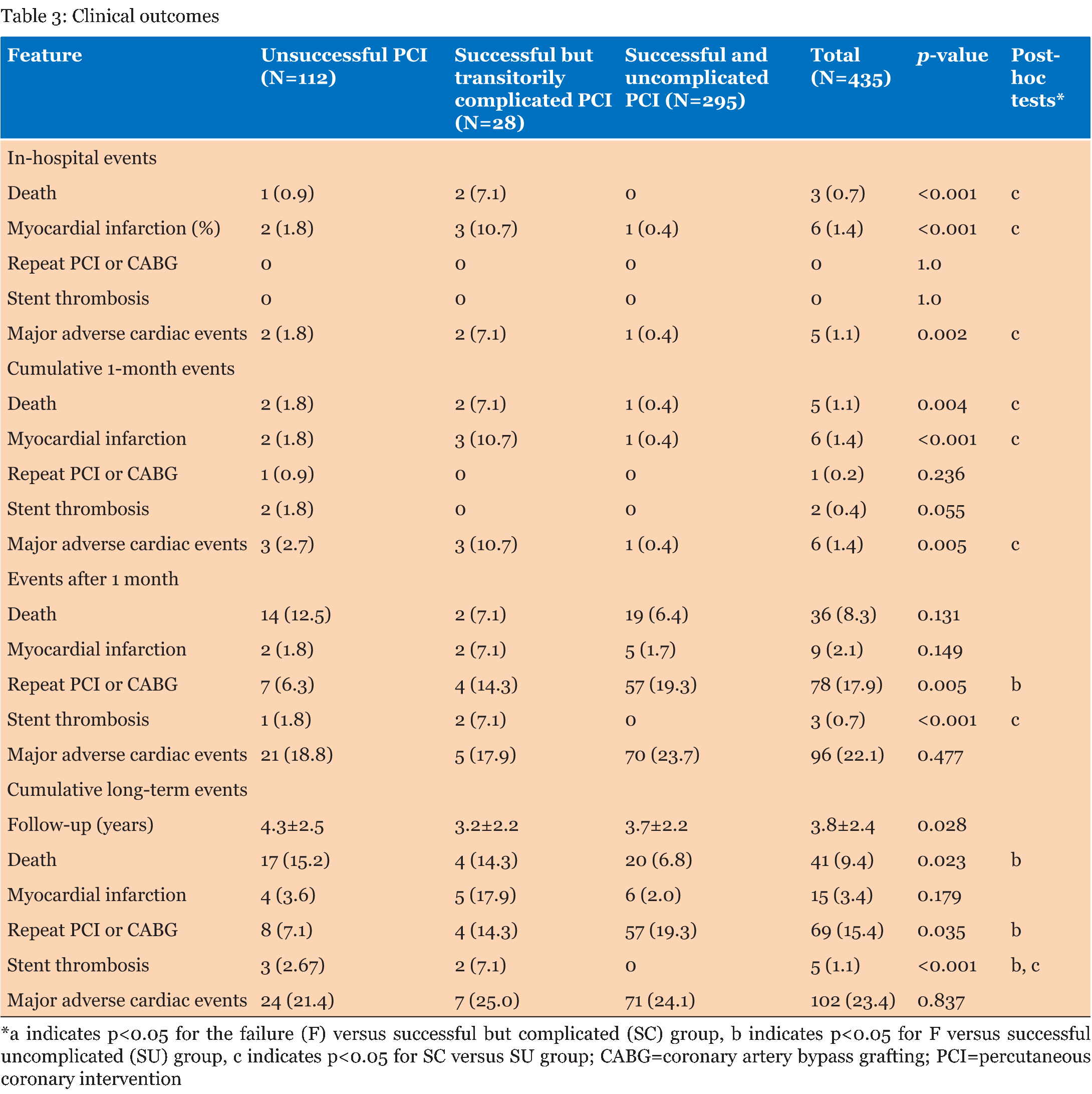
Between January 2003 and June 2012, 435 patients with at least 1 CTO lesion underwent PCI in our institution, with 112 (25.7%) in the F group and 323 (74.3%) successes, including 28 (6.4%) in the SC group and 295 (67.8%) in the SU group (Table 1). Success rates increased over time from 66.8% in the first five years to 80.1% in the last five years of the series (p<0.001), whereas the complication rate remained stable over time (9.8% versus 8.2%, p = 0.342) (Figure 1A-B). Most baseline features were similar across the groups with a higher prevalence of male sex in all the groups (89 [79.4%] in F group, 24 [85.7%] in SC group and 239 [81.0%] in SV group, p 0.751). However, patients in the F group were older than those from the other groups (67.7±9.1 years versus 64.0±11.1 years in the SC group versus 65.4±9.1 years in the SU group, p = 0.047). Conversely, patients in the SC group had a higher prevalence of prior CABG (3 [10.7%] versus 6 [5.4%] in the F group versus 1 [0.3%] in the SU group, p<0.001). Angiographic and procedural features are reported in Table 2. Retrograde tracking, in general, was used more frequently in the SC group (7 [25.0%] versus 11 [9.8%] in the unsuccessful PCI group versus 15 [5.1%] in the SU group, p < 0.001), as was septal tracking, in particular (respectively 6 [21.4%] versus 9 [8.0%] versus 14 [4.7%], p = 0.003), and intravascular ultrasound imaging (5 [17.9%] versus 2 [1.8%] versus 31 [10.5%], respectively, p=0.004). Conversely, contralateral injection had been used more commonly in the SU PCI group (75 [25.4%] versus 13 [11.6%] in the F group versus 3 [10.7%] in the SC group, p=0.004). Notably, drug-eluting stenting was more common in the SC group (21 [75.0%] versus 191 [64.7%] in the SU group versus 9 [8.0%] in the F group, p<0.001), with accompanying longer total stent length (56.6±26.2 mm versus 43.6±23.8 mm versus 35.6±22.2 mm, respectively, p < 0.001). Intravascular ultrasound was used also more commonly in such patients (5 [17.9%] versus 31 [10.5%] versus 2 [1.8%], respectively, p=0.004). Most common reasons for procedural failure included inability to cross the lesion with the wire (27 [24.1%]) and inability to cross the lesion with a larger device despite successful wire deployment (9 [8.0%]). Detailed analysis of peri-procedural complications, excluding according to this work premises the SU group, showed that the most common complication was minor perforation (13 [3.0%]). Clinical outcomes are described in Table 3. In-hospital death was significantly more common in the SC group (2 [7.1%] versus 1 [0.9%] in the F group versus 0 in the SU group, p<0.001), with similarly increased risks of myocardial infarction (3 [10.7%] versus 2 [1.8%] versus 1 [0.4%], p<0.001) and MACE (2 [7.1%, versus 2 [1.8%] versus 1 [0.4%], p=0.002). Similar results were still evident at cumulative one month follow-up (2 [7.1%] versus 2 [1.8%] versus 1 [0.4%], p =0.004, 3 [10.7%] versus 2 [1.8%] versus 1 [0.4%], p < 0.001 and 2 [7.1%] versus 3 [2.7%] versus 1 [0.4%], p 0.005) respectively. Conversely, after 1 month the groups showed similar rates of death (2 [7.1%] versus 14 [12.5%] versus 19 [6.4%], p=0.131), myocardial infarction (2 [7.1%] versus 2 [1.8% versus 5 [1.7%], p=0.149) and MACE (5 [17.9%] versus 21 [18.8%] versus 70 [23.7%], p = 0.477), but with a higher rate of stent thrombosis in the SC group (2 [7.1%] versus 1 [1.8%] in the F group and 0 [0.0%] in the SU group, p <0.001) and a higher need for revascularization in the SU group (56 [19.3%] versus 4 [14.3%] in the SC group and 7 [6.3%] in the F group, p=0.005). Cumulative long-term follow-up showed a higher death rate in the SC group (4 [14.3%]) and in the F group (17 [15.2%]) in comparison to the SU group (20 [6.8%], p=0.023), higher stent thrombosis rate in the SC group (2 [7.1%] versus 3 [2.67%] in the F group and 0 in the SU group, p<0.001) and a higher need for revascularization in the SC group (4 [14.3%]) and in the SU group (57 [19.3%]) in comparison to the F group (8 [7.1%], p=0.035). Computation of failure curves with the Kaplan-Meier method and their comparison with the log-rank test did not confirm however a statistically significant difference in the risk of death when comparing the different groups (Figure 2), whereas it confirmed the similar cumulative risk of MACE in the F, SC, and SU group (Figure 3), despite persisting trends in favor a better outlook for patients in the SU group. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
The main findings of this large single-center registry on percutaneous coronary recanalization of CTO lesions are:
Percutaneous CTO recanalization remains a challenging procedure with relatively low success rate of approximately 70–85% [6] [12] [13] [15], and with extremely variable results among operators [3]. Recently, Thompson et al. showed that operator expertise is very important for successful CTO recanalization [16]. Specifically, operators who are not experienced in retrograde techniques were successful in recanalizing a CTO in 58.9% of the cases, while retrograde operators presented a success rate of 75.9%. Importance of experience and evolution in techniques and materials is also underlined in a recent publication analyzing Japanese experience with an increase in successful procedures from 80% up to 90% in a few years [12]. European operators showed similar trends despite some differences in approach [13]. Despite a more aggressive approach major complications remain generally uncommon. Death is a rare complication (0.2–1.3%) [3] [15], and similar trends for non-CTO PCI are showed by periprocedural myocardial infarction (0.2–0.5%), emergency CABG and periprocedural MACE [3] [12][15][17]. In our experience successful recanalization increased from 66.8–80.1%. These are results of a center with a specific CTO program accomplished by experienced operators with full understanding of technology and techniques related with CTO procedures and able, when indicated, to expertly perform retrograde CTO PCI. The overall risk of CTO PCI complications has been assessed in several studies. Major adverse cardiac event rates are similar to non-CTO patients (on average 3.8%), with a death rate of 0.2–1%, Q-waves myocardial infarction of 0.2–2.5%, urgent coronary artery bypass surgery in <1% [3] [7][15][17], but CTO PCI still presents a higher rate of specific complications such as vessel dissection and coronary perforations [18] [19]. In particular, coronary perforations is reported in 0.9–7.2% of cases [17] [20], are related with cardiac tamponade and procedural failure [6] [15], but without an adverse prognosis at follow-up [12]. Coronary perforation has been the most frequent complication in our population. Minor perforations were detected in 3.0% and vessel rupture in 0.5%; pericardial drainage was performed in 1.1% and covered stent or coil embolization in 1.0%. In the majority of cases, minor perforations were not considered a reason to abort the procedure and PCI was successfully completed even after more aggressive maneuvers. Donor vessel dissection was reported in 0.5% and in all the patients the procedure was concluded with successful recanalization. In-hospital events are similar to previously reported data for the non-CTO PCI population, with a 0.7% death rate and a 1.1% MACE rate, with a higher incidence in the group of successful albeit complicated recanalization CTO, despite a similar trend after one month. At follow-up unsuccessful PCI was conversely related with higher mortality, while patients with successful PCI experienced a higher rate of stent thrombosis (1.1%) and repeated revascularization (15.4%). The latest is higher than previously reported [7] and can be partially explained by the relatively low drug eluting stent (DES) utilization (50.8%). In fact, it is well known that DES can reduce both TVR and target lesion revascularization [8] [21], without a concomitant increase in the risk of stent thrombosis [8]. In our experience, stent thrombosis rate was lower than what was reported in other series (Mehran) with a higher incidence in the successful but transiently complicated group. This result could suggest a specific benefit for prolonged and more aggressive dual antiplatelet therapy in this subgroup, but more robust evidence from randomized trials is necessary. This work is limited by the observational, retrospective, and single-center design. Other limitations include the examined period which reflects different level of experience by the operators and different techniques and devices avoidable for the procedure and the absence of pre specified criteria to stop the procedure, particularly in presence of complications. | ||||||
|
Conclusion
| ||||||
|
In conclusions, the rate of procedural success in percutaneous coronary intervention (PCI) for chronic total occlusion (CTO) is frequent and has increased in the last few years without a consequent increase in periprocedural complications. Patients with uncomplicated recanalization may be at higher risk of restenosis and repeat revascularization, whereas those with final success despite procedural complications may be at higher risk of stent thrombosis. These findings are important to tailor monitoring and secondary prevention strategies in CTO patients. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Andrea Gagnor – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ferdinando Varbella – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Francesco Tomassini – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Sara Giolitto – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Cristina Rolfo – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Emanuele Tizzani – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Enrico Cerrato – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Alfonso Gambino – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Elisa Favro – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Rosario Tripodi – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Maria Cristina Rosa Brusin – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Paolo Gyai Pron – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Mariangela Peruzzi – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Giuseppe Biondi-Zoccai – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Andrea Gagnor et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|