| Table of Contents |  |
|
Original Article
| ||||||
| Impact of sex on the early and long-term outlook of patients undergoing carotid artery stenting with a single embolic protection device-stent combo | ||||||
| Arturo Giordano1, Paolo Ferraro1, Nicola Corcione1, Michele Polimeno1, Stefano Messina1, Gabriele Giordano1, Rosario Mancusi1, Raffaella Avellino1, Giacomo Frati2, Giuseppe Biondi-Zoccai2 | ||||||
|
1Unità Operativa di Interventistica Cardiovascolare, Presidio Ospedaliero Pineta Grande, Castel Volturno, and Unità Operativa di Emodinamica, Casa di Salute Santa Lucia, San Giuseppe Vesuviano Italy.
2Department of Medico-Surgical Sciences and Biotechnologies, Sapienza University of Rome, Latina, Italy. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Giordano A, Ferraro P, Corcione N, Polimeno M, Messina S, Giordano G, Mancusi R, Avellino R, Frati G, Biondi-Zoccai B. Impact of sex on the early and long-term outlook of patients undergoing carotid artery stenting with a single embolic protection device-stent combo. Edorium J Cardiol 2015;2:9–15. |
|
Abstract
|
|
Aims:
Whether men and women benefit similarly from carotid artery stenting (CAS) remains uncertain. We hypothesized that CAS, especially when performed with the same combination of embolic protection device (EPD) and stent, may have a different risk-benefit profile in men and women.
Methods: We retrospectively collected data on all patients undergoing CAS with the Angioguard EPD and Precise RX stent. A total of 447 patients were included, 285 (64%) men and 162 (36%) women. Results: Despite several baseline, lesion and procedural differences, procedural success and clinical outcomes were similar (all p > 0.05), at both discharge and long-term follow-up (19±21 months). Specifically, the composite of death, myocardial infarction, stroke or transient ischemic attack occurred in 5 (2%) men and 2 (1%) women at discharge, and 32 (11%) men and 12 (7%) women at follow-up (both p > 0.05). Even after propensity score matching, no significant differences were found (all p > 0.05). Conclusion: In conclusion, despite several baseline disparities, there are no differences in the early and long-term incidence of adverse events in men versus women undergoing CAS. | |
|
Keywords:
Carotid artery disease, Carotid artery stenting, Gender, Sex, Stroke
| |
|
Introduction
| ||||||
|
Carotid artery disease is a common cause of ischemic stroke, with important ensuing consequences on life quality and expectancy. Carotid artery stenting (CAS) has been proven equivalent to the surgical reference standard, i.e., carotid endarterectomy, especially in patients at high surgical risk, but inconsistent results have been reported in some trials [1][2]. Sex may impact on many pathophysiological processes, disease features, and comorbidities, and the precise role of sex on the risk of carotid artery disease and the comparative benefit of CAS has been questioned repeatedly [3]. In particular, a number of trials have suggested that women appear to have a lower likelihood of benefit from carotid endarterectomy (CEA), and similar findings have been reported in a subset of studies on CAS [3] [4][5]. Since inception, it has been hallmark of our practice to use a single embolic protection device-stent combination (respectively Angioguard and Precise Rx, both from Cordis, Natick, MA, USA) in most (>80%) of our carotid PTAs [6]. Accordingly, we have accrued a substantial expertise in using these devices. We hypothesized that we could exploit this common therapeutic ground to perform a more informative, accurate and precise comparison of the baseline, procedural and outcome features of men versus women undergoing CAS, under the premises that indeed women may benefit less than men from CAS. | ||||||
|
Materials and Methods
| ||||||
|
This was a retrospective observational study stemming from our comprehensive administrative database registry, for which the competent ethics committees have been notified in keeping with Italian regulations and for which patients provided written informed consent. Specifically, we queried our Cardioplanet (Ebit, Genova, Italy) database for all patients undergoing percutaneous transluminal angioplasty (PTA) for carotid stenosis at our institutions with attempted use (irrespective of success) of the Angioguard-Precise Rx combo. From the initial sample of 532 patients, we excluded cases in which only the Angioguard device (N=2), only the Precise Rx device (N=73), or neither (N=10) had been used, yielding a total of 447 patients, notwithstanding that choice of technique and device were at the operator's discretion. All patients underwent preliminary carotid angiography followed by PTA or CAS as appropriate. Specifically, subjects without prior stroke or transient ischemic attack (TIA) were treated if showing a diameter stenosis >60%, whereas symptomatic patients were treated if showing a diameter stenosis >50% [7]. All devices were used according to their instructions for use, unless in bailout conditions. Carotid revascularization was typically performed as follows: after diagnostic angiography, a 7 French 11 cm sheath was exchanged (Cordis) and a 7 French JR4 guiding catheter was deployed tracking over an Amplatz Super stiff 0,035" guidewire (St. Jude Medical, Minneapolis, MN, USA) previously deployed in the common carotid artery. Through the guiding catheter, the Angioguard was deployed. Predilation was performed after deployment of the Angioguard sparingly and only when deemed appropriate, using an undersized balloon (typically 3.0x20 mm). The Precise Rx stent was then deployed, and always post-dilated with a slightly undersized balloon (typically 5.0x30 mm). Antithrombotic therapy encompassed unfractionated heparin (70 IU/kg) plus further boluses depending on procedure duration and provisional tirofiban IV bolus (at a dose ½ to ½ of the one approved for percutaneous coronary intervention) in case of complex patient or lesion features [8]. Antiplatelet therapy consisted in aspirin and a thienopyridine for at least 3 days before the procedure, or 250 mg aspirin IV bolus and/or clopidogrel 300 mg front-loading in those not pre-treated. After PTA or CAS, all patients were prescribed aspirin 100 mg qd and clopidogrel 75 mg qd for at least one month. The primary outcome of interest of this work was the composite of death, myocardial infarction (MI), stroke or transient ischemic attack (TIA). Other outcomes included the individual components of the composite endpoint, the composite of death, myocardial infarction, or stroke, the composite of death or stroke, hospital stay, and repeat revascularization. All outcomes were adjudicated in-hospital and at long-term. Continuous variables are reported as mean and categorical variables as n (%). Continuous variables were compared with unpaired t-test, categorical variables with Fisher exact test, and censored variables with the log-rank test. In order to adjust for potential confounders, [9] propensity matching was performed with a 1:1 men to women ratio and a caliper corresponding to 0.001 of the logit of the probability of being female (Online Supplement). After propensity matching, key outcomes were compared with conditional logistic regression or shared Cox proportional hazard analysis in order to take into account the clustering features, with Fisher exact testing also used for sensitivity analysis. Computations were performed with Stata 13 (StataCorp, College Station, TX, USA). | ||||||
|
Results | ||||||
|
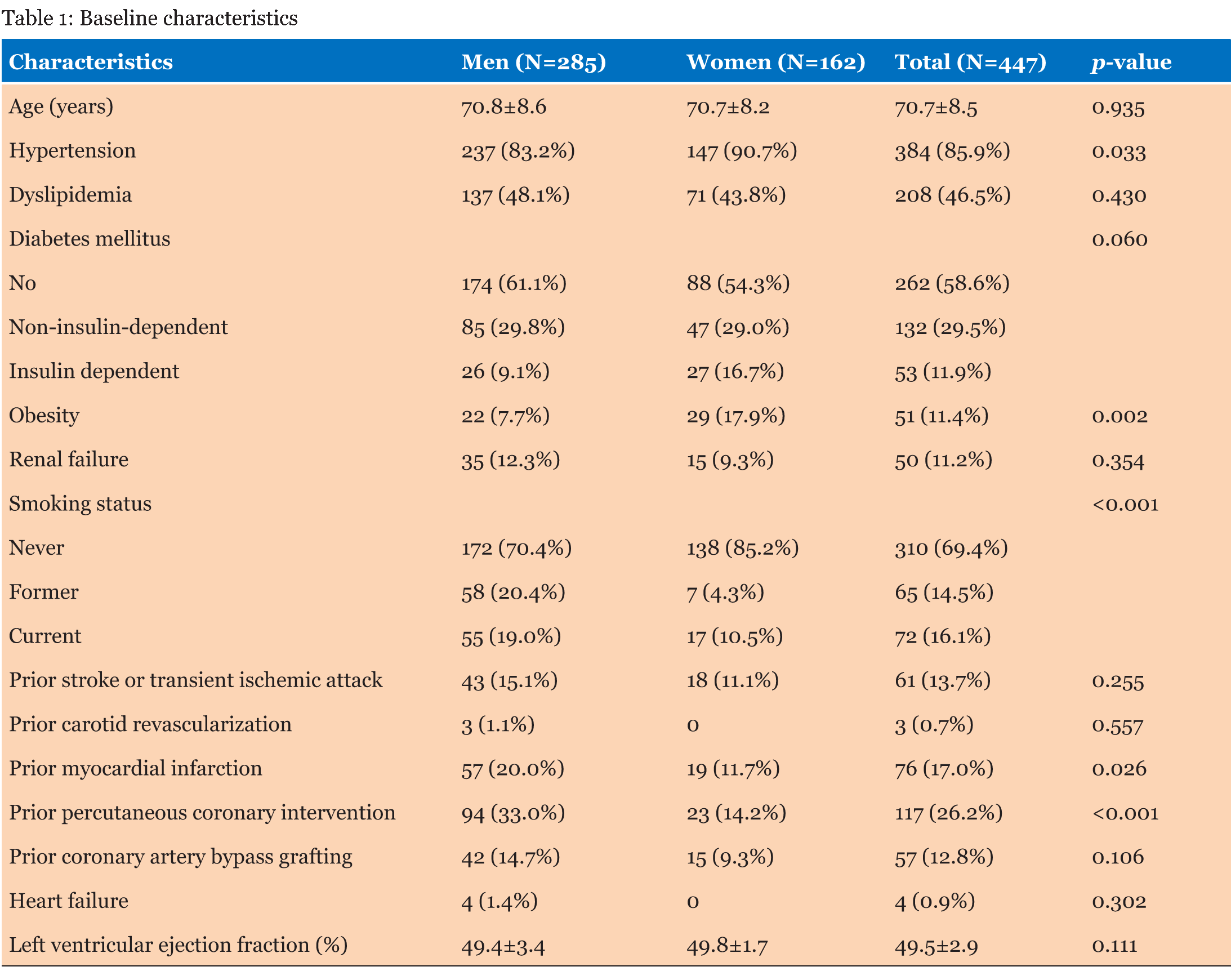
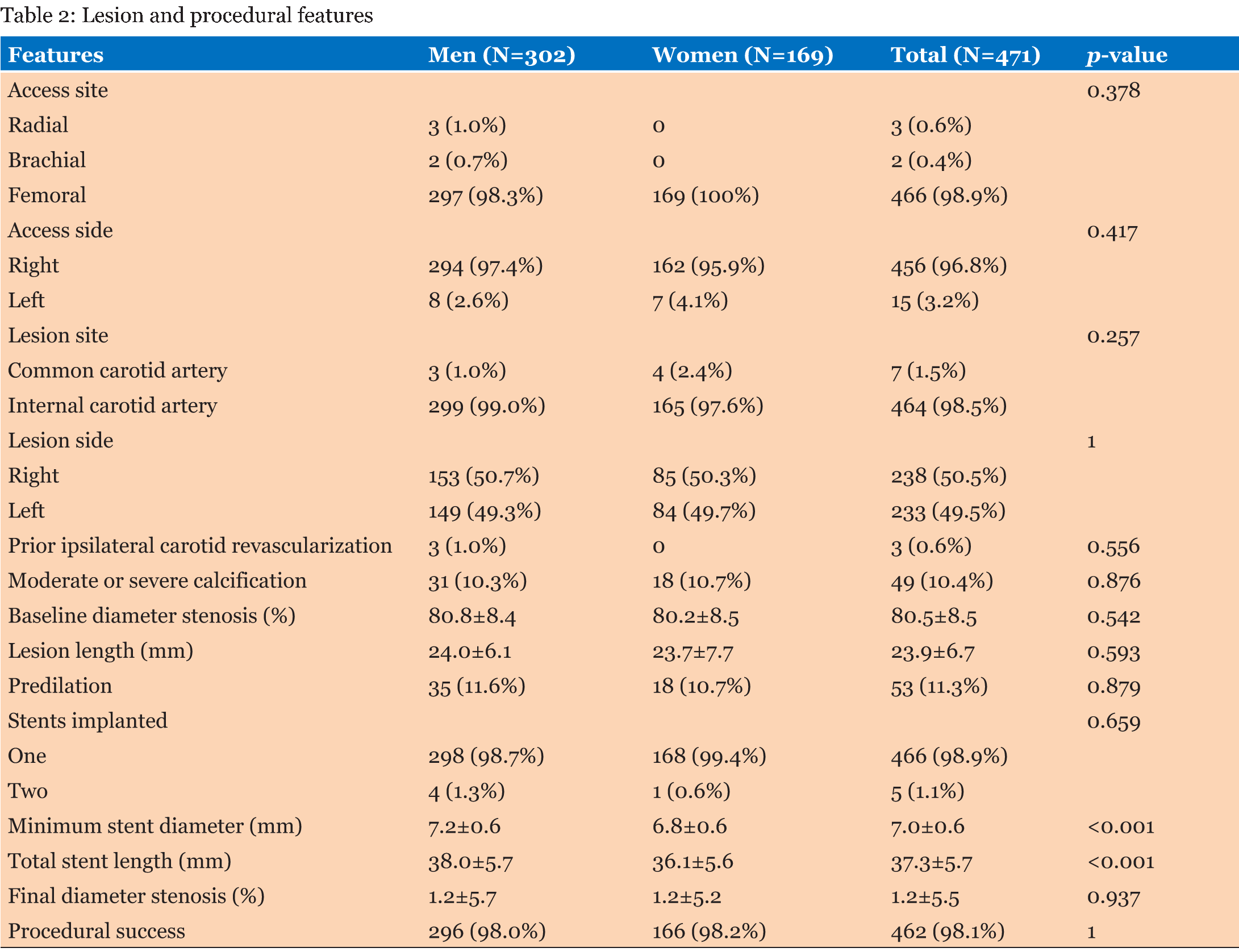
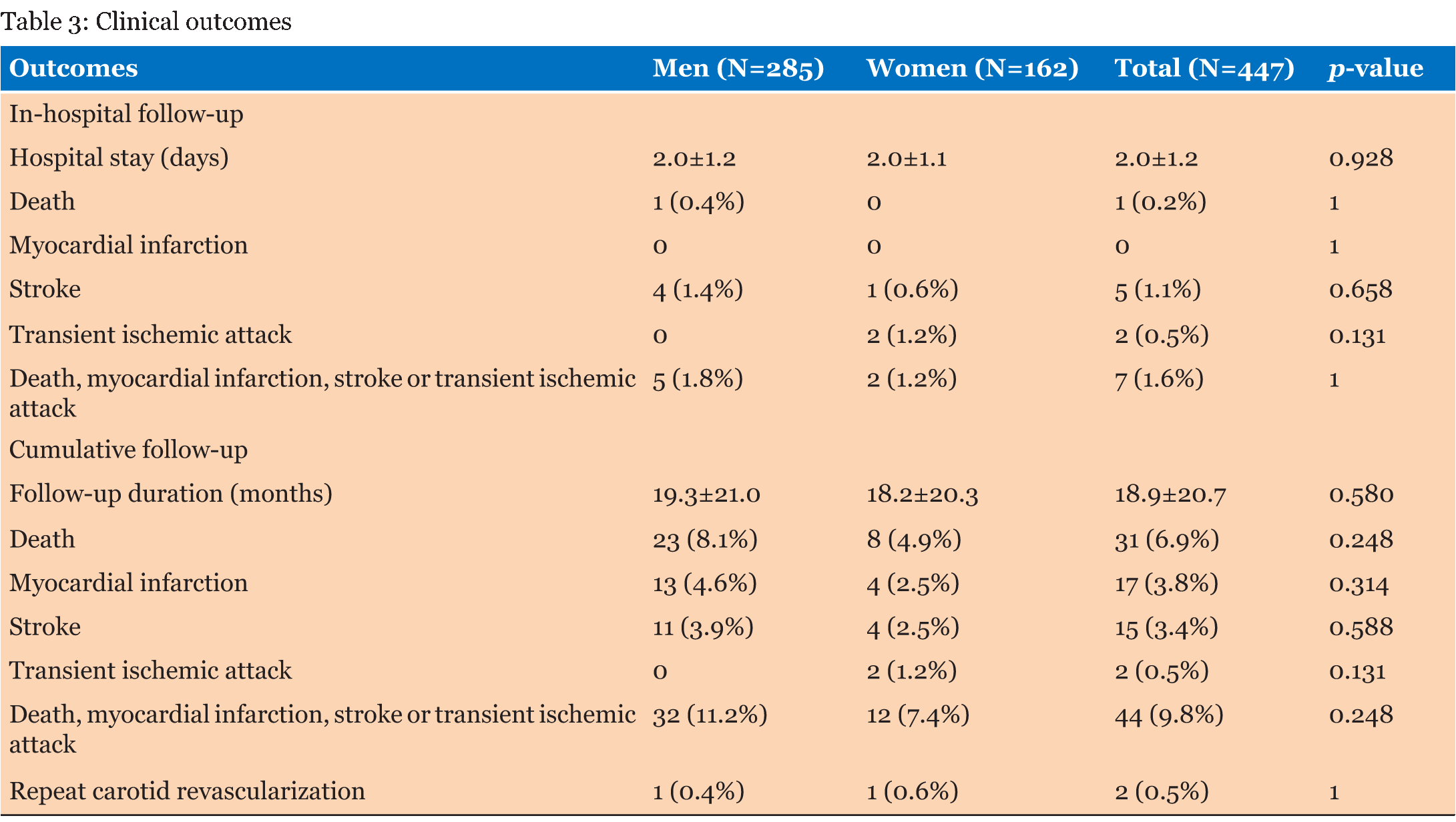
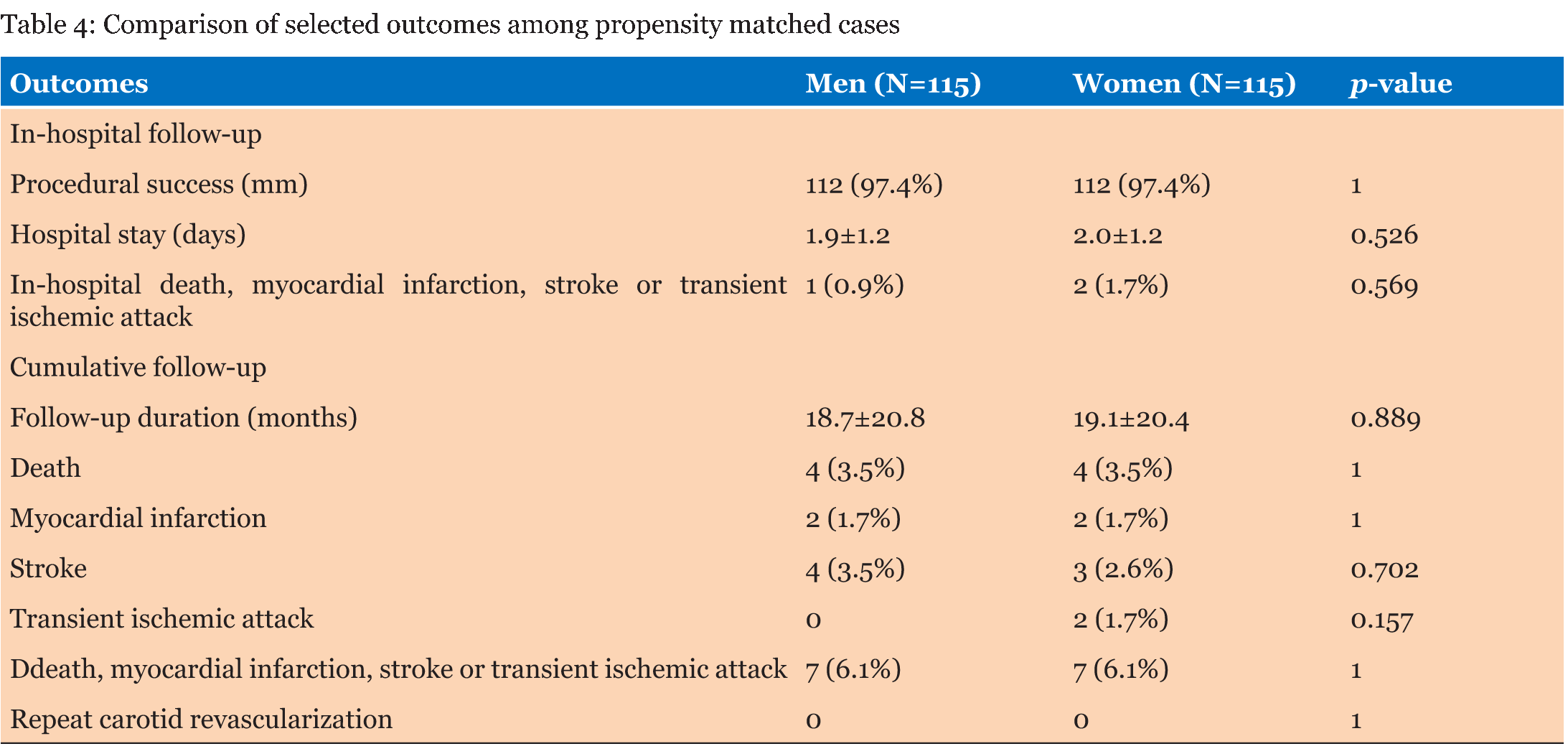
We included 285 (63.8%) men and 162 (36.2%) women, for a total of 447 patients, most (86%) of them being asymptomatic (Table 1). Baseline features were largely similar, with the notable exception of higher prevalence of hypertension (p=0.033) and obesity (p=0.002) in women, and a greater likelihood of history of smoking (p<0.001), prior myocardial infarction (p=0.026), and prior percutaneous coronary intervention (p<0.001) in men. Conversely, no significant differences were found for age, diabetes mellitus, renal failure, prior stroke or TIA, prior carotid revascularization, prior coronary artery bypass grafting, heart failure or systolic function (all p>0.05). A limited set of sex-related differences in lesion and procedural features were found (Table 2). Specifically, stent diameter was larger (p<0.001) and total stent length longer (p<0.001) in men. Conversely, no significant differences were found for access site, access side, lesion site, lesion side, prior ipsilateral carotid revascularization, calcified lesion, baseline diameter stenosis, lesion length, predilation, number of stents, final diameter stenosis or procedural success, which was achieved in 296 (98.0%) lesions in men and in 166 lesions (98.2%) in women (all p > 0.05). Clinical outcomes were similar at unadjusted analysis in men and women during the index hospital stay and also after 18.9±20.7 months of cumulative follow-up (Table 3). In particular, no significant difference was found for the risk of death, MI, stroke, TIA or their composite, for the risk of repeat revascularization, or for hospital stay (all p > 0.05). After propensity matching, a total of 230 cases were shortlisted with closely similar (0.001 caliper) propensity scores (115 men and 115 women; Table 4; Figure 1). No significant differences were found comparing males and females even in such homogenous subset of cases, with procedural success in, respectively, 112 (97.4%) versus 112 (97.4%, p=1), and death, myocardial infarction, stroke or transient ischemic attack in 1 (0.9%) versus 2 (1.7%, p=0.571) at hospital discharge and in 7 (6.1%) and 7 (6.1%, p=1) at long-term follow-up. Finally, both unadjusted and propensity-adjusted survival analyses for the risk of death, MI, stroke or TIA confirmed the lack of significant differences between men and women (p>0.05 for both; Figure 1). | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
|
| ||||||
|
Discussion
| ||||||
|
This retrospective observational study focusing on sex-related differences in mostly asymptomatic patients undergoing CAS with a single EPD-stent combination suggests that there are no significant differences between men and women at either short-term or long-term follow-up, even adjusting for baseline and procedural differences. The topic of gender-related differences in patients undergoing CAS is a particularly important one, as it stands to reunite two apparently distant issues capable of strongly interesting clinicians and researchers. Indeed, the impact of sex on cardiovascular disease has always been of great interest to scientists as well as practitioners [10]. First, because such sex-based distinction is a simple and immediate way of characterizing patients. Second, because gender strongly correlates with many other important risk features, and thus may be a reasonably accurate yet practical proxy for risk assessment. Third, and most likely most importantly, highlighting and understanding differences between genders in cardiovascular medicine may lead to better understanding and treating cardiovascular disease irrespective of gender itself. Indeed, gender-related issues in cardiovascular medicine have already been the focus of intense research from our own group [11]. Among our recent contributions is the pathologic analysis of CEA specimens focusing on the comparison of men versus women [12]. In this recent work, we highlighted that that apparently thrombotic plaques were less common in females, with concomitant lower percentage area of necrotic core and hemorrhagic extension. In addition, women seemed to have a lower concentration of inflammatory cells and macrophage foam cells in the plaque cap. Yet, such differences did not hold true after multivariable adjustment, suggesting that they were simply due to differences in baseline patient features and risk profiles. Building upon such premises and other works that have suggested that women may fare differently (actually worse) than men when undergoing CEA or CAS, we aimed to exploit our unique practice pattern of using for most procedures a single EPD-stent combo, and compare in such uniform setting the outlook of CAS in the two genders. We found that several differences were evident in baseline and procedural features, with women having a higher prevalence of hypertension and obesity, but a lower prevalence of smoking history, prior myocardial infarction, prior percutaneous coronary intervention. In addition, average stent diameter and length were lower in women. Despite such differences, and possibly in light of a 14% prevalence of symptomatic carotid disease, no significant difference was found in men versus women for the risk of death, MI, stroke, TIA, or other clinically relevant endpoints. Even after propensity matching, no significant difference was found in short-term or long-term events when comparing men versus women. While our work conflicts with reports suggesting the impact of gender of the outcome of CAS, [5] [13][14]other studies have provided similar findings for men and women undergoing CAS, such as Park et al., [15] and Jim et al. [16]. Indeed, the scientific literature is rich of settings in which the impact of gender on clinical outcomes is hotly debated, with some studies suggesting that gender may play a significant and independent role, and other discounting such scenario. Indeed, while there are several reasons that support the fact that women may respond to CAS differently than men (e.g., Y-linked conditions or factors, hormonal differences, risk profile differences), other counterarguments may be proposed. Accordingly, significant differences between females and males in the previously quoted studies could still be due to residual and unaccounted for confounding (this especially holds true for retrospective studies based on administrative datasets, where information bias is always possible). This work has several limitations, including the retrospective design and the inherent selection bias due to the focus on patients treated only with the same EPD-stent combo. In addition, no core lab analysis of imaging (ultrasound, angiography) data was performed. Finally, specific details on menopause or hormonal therapy, which would have been interesting for the female group, could not be retrieved from our database. | ||||||
|
Conclusion
| ||||||
|
The present series of mostly asymptomatic patients undergoing carotid artery stenting (CAS) with a single EPD-stent combination suggests that, despite several baseline, lesion and procedural disparities, there are no differences in the early and long-term incidence of adverse events in men versus women. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Arturo Giordano – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Paolo Ferraro – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Nicola Corcione – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Michele Polimeno – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Stefano Messina – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Gabriele Giordano – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Rosario Mancusi – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Raffaella Avellino – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Giacomo Frati – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Giuseppe Biondi-Zoccai – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Arturo Giordano et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|